Let’s Discuss Smarter Value-Based Care at APG 2026

The statistics are striking. The 476 ACOs participating in the Medicare Shared Savings Program saved $4.1 billion in 2024, a record high since the program began. Importantly, physician-run organizations tend to perform better than those that are led by hospitals. Full risk capitation works the same way. Those ACOs that possess the necessary infrastructure end up in the lead, while others try to catch up for most of the time.
If you're heading to the
APG Spring Conference 2026 in San Diego, that context probably feels familiar. This year's theme, "Delivery, Dollars, and Determination: Challenges and Opportunities in Accountable Care," addresses the challenge that physician groups, IPAs, and MSOs navigate every single day. Delivering better care while staying financially sustainable takes more than clinical intent. It takes operational machinery that actually works.
MedVision will be at Booth #618 from May 27 to May 29 at the Marriott Marquis San Diego Marina, bringing QuickCap 7 to a room full of the people running some of the country's most sophisticated physician-led organizations. If you want to see what purpose-built physician group management software looks like in practice, that's where we'll be.
See How Physician Groups Operate Smarter
The Physician Group Landscape in 2026
America's Physician Groups represents approximately 340 physician group members, collectively comprising nearly 260,000 physicians and other clinicians who care for close to 90 million patients, including roughly 1 in 4 Americans and 1 in 3 Medicare Advantage enrollees. That's not a niche market. It's the backbone of value-based care administration in the United States.
There is increasing pressure on those organizations in that network. The level of complexity in terms of risk arrangements is higher now than it was five years ago. In addition, CMS continues to grow in terms of accountable care objectives, including the highest savings through MSSP participation for 2024, as well as the use of two-sided risk programs. Medicare Advantage enrollment continues to rise, creating an even greater administrative burden for physicians.
What makes the difference now isn’t that physicians aren’t aware of what value-based care entails. That’s well-known among the executives involved in such care at this point. The difficulty comes with implementation: ensuring networks stay cohesive, claims management runs smoothly, utilization remains controlled, and the data required to run the business isn’t scattered across four separate systems.
Where Physician Groups Are Lagging Ground Operationally
Organizations having difficulty operating under value-based agreements tend to share a common denominator: their organizational framework is outdated relative to the current healthcare model. While fee-for-service processes scale well in the former system, once you move towards full risk, those processes become liabilities due to the shift from volume to value. This is where the conflicts arise.
Capitation Reconciliation That Happens Manually
When capitation payments come in from multiple health plans, each with its own file format, frequency, and reconciliation requirements, the back-office burden compounds fast. Organizations spending hours on manual capitation processing are diverting resources away from care management and compliance. A true capitation management platform handles this automatically, yet many physician groups and IPAs are still working around workarounds.
Referral Leakage With No Early Visibility
Out-of-network referrals are one of the most consistent ways physician groups leave value on the table under capitated or shared-savings arrangements. If your team isn't seeing referral patterns in real time, you're not managing the network; you're reporting on it. By the time the data surfaces, the opportunity to intervene has already passed.
Claims Workflows That Create Downstream Errors
In a capitation environment, claims adjudication accuracy matters not just for revenue, but for encounter data accuracy, quality measurement, and regulatory compliance. Manual processes at this stage introduce errors that ripple outward into reporting, risk adjustment, and audit exposure. In a two-sided risk arrangement, those errors have direct financial consequences.
Population Data That Doesn't Drive Action
Most organizations have some form of population data. What separates high performers from the rest is whether that data is actionable in real time or just a quarterly snapshot that arrives too late to change anything. Without the right managed care workflow automation, even good data sits idle.
How QuickCap 7 Addresses These Challenges Head-On
MedVision has been building healthcare administration software since 1994. QuickCap 7 (QC7) isn't a general-purpose practice management tool that physician groups are expected to adapt to; it was designed from the ground up for the operational reality of risk-bearing organizations: IPAs, MSOs, physician-hospital organizations (PHOs), ACOs, TPAs, and the hybrid structures that don't fit neatly into any one category. Here's what that looks like in practice for the organizations that matter most at APG.
Capitation Management and Multi-Payer Reconciliation
Managing capitation across multiple health plans is one of the most administratively intensive tasks a physician group faces. As a true capitation management platform, QC7 supports loading enrollment, eligibility, revenue, and capitation files according to each health plan's frequency and format. Reconciliation happens inside the system rather than through separate tools or manual processes, reducing the back-and-forth that typically drags out month-end close cycles. For organizations running multiple lines of business across different payers, centralizing this function significantly changes the dynamic.
You can read more about how this translates to better patient outcomes in our overview of
how capitation drives better results in value-based care.
Claims Auto-Adjudication with Custom Rules
QC7 supports rule-based claims auto-adjudication built around each payer's specific requirements. Custom rules drive routing decisions, reduce manual review volume, and accelerate the revenue cycle without requiring additional headcount. Encounter processing and submission to health plans is built into the workflow, ensuring network performance data stays accurate and timely. In a capitation environment, that kind of throughput consistency matters every single month.
Referral and Authorization Management
Out-of-network leakage doesn't have to be discovered quarterly. QC7's referral management tools give your team real-time visibility into inbound and outbound referral patterns, with configurable routing rules that keep patients within the preferred network when clinically appropriate. Authorization management works the same way: custom rules reflect your clinical and financial policies rather than a one-size-fits-all default logic. The result is faster approvals, fewer manual touchpoints, and utilization management that stays aligned with your cost and quality targets.
For a closer look at how this supports IPA-specific workflows, see our piece on
improving operations for your value-based IPA.
Population Health Dashboards and Reporting
Value-based care administration runs on visibility. QC7 includes customizable executive-level dashboards that surface utilization trends, cost performance, and quality metrics in a format decision-makers can act on. Quality and utilization reporting is built directly into the platform, which means your team spends less time pulling data and more time responding to what it shows. When the right information reaches the right people at the right moment, operational decisions tend to improve as well.
EDI Data Management and Network Interoperability
QC7's embedded Electronic Data Interchange (EDI) functionality handles data movement across the network without requiring manual file management. This is particularly relevant for independent physician association software use cases, where organizations need to maintain provider records, contract alignments, and upstream/downstream arrangements with multiple health plan partners simultaneously. Consistent data flow reduces communication gaps, keeps compliance documentation current, and ensures that encounter data reaches health plans on time.
For a broader view of what QC7 looks like in a fully operational
IPA environment, explore our IPA software and network management solution page.
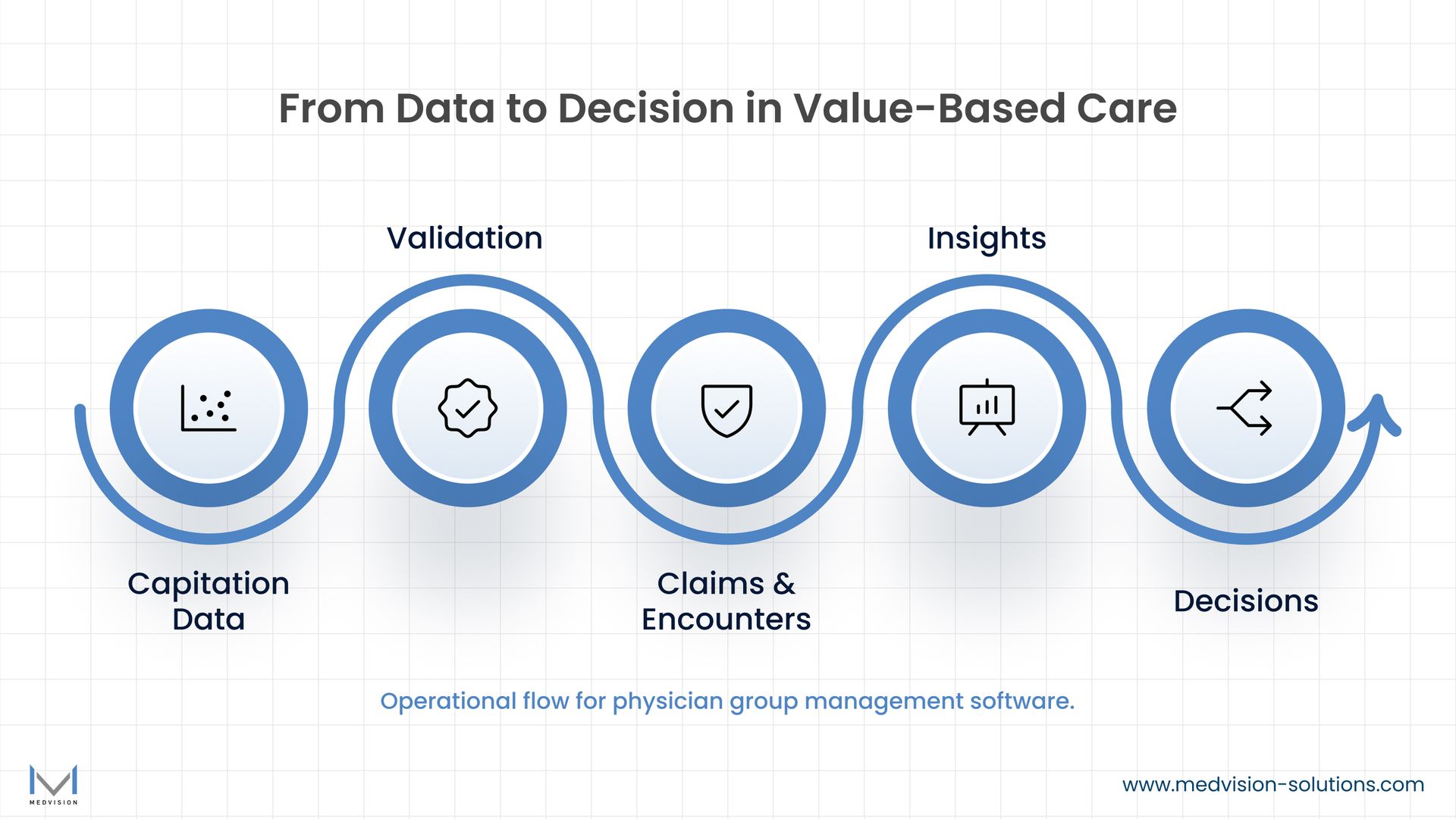
What the APG Spring Conference Represents for the Physician-Led Care Community
APG Spring Conference is not merely a networking opportunity; it is a place where the folks who actually run the physician practices, IPAs, and MSOs meet and exchange ideas, discuss successes, and decide on their future plans. The conference theme for 2015, "Delivery, Dollars, and Determination: Challenges and Opportunities in Accountable Care," makes this point quite clearly. Providing care through a value-based model is not only a policy issue; it is a practical task that requires determination and money.
APG's membership includes organizations at every point along the value-based care continuum, from groups just beginning to take on risk to mature capitation-based organizations managing full-risk arrangements across Medicare Advantage, MSSP, Medicaid, and commercial populations. The conversations at this conference reflect that range, and so does the technology that those organizations actually need. Physician-led ACOs, in particular, have proven that their model generates stronger results, a point APG's own research has consistently underscored, but sustaining that performance requires physician group management software that can keep pace with the demands.
MedVision has been at this intersection since 1994. Our team will be at Booth #618 throughout May 27-29 for one-on-one conversations and platform walkthroughs. Whether you're evaluating a new system for the first time, looking to replace a platform that's showing its limits, or just curious what QuickCap 7 looks like in your specific organizational context, stop by and let's talk through it.
Coming to APG Spring 2026? Here's How to Find Us
Event:
APG Spring Conference 2026
Theme:
Delivery, Dollars, and Determination: Challenges and Opportunities in Accountable Care
Dates:
May 27-29, 2026
Location:
Marriott Marquis San Diego Marina, San Diego, CA
MedVision Booth:
#618
The conference brings together physician group leaders, clinical directors, IPA and MSO administrators, payer executives, and healthcare innovators from across the country. If value-based care is central to how your organization operates, this is the room to be in. Stop by Booth #618 anytime during the event, or explore our
QuickCap solutions page ahead of time to get a sense of what we'll be walking you through.
Let's Talk at APG 2026
Frequently Asked Questions
What is physician group management software, and how does it differ from standard practice management tools?
Common practice management systems primarily emphasize scheduling, billing, and EHR within a single clinical location. A physician group management system, however, is far more extensive and includes capitation processing, multi-payor claims processing, referrals, authorization, population health metrics, and quality reports, among others. This software is intended to meet the needs of risk-taking organizations rather than practice management per se.
How does independent physician association software support full-risk capitation models?
Full-risk capitation requires accurate enrollment/eligibility, capitation reconciliation based on payer and encounter data, encounter data reporting, and utilization management across a large, diverse attributed population. An IPA-centric software solution, such as QuickCap 7, integrates all of these capabilities into a singular and customizable application, thereby eliminating inefficient standalone systems that generate overhead.
What does managed care workflow automation actually do for day-to-day operations?
At its core, managed care workflow automation reduces the number of manual steps between incoming data and actionable decisions. For physician groups and IPAs, this means auto-adjudication of claims using custom payer rules, automated routing of referrals and authorizations, real-time dashboard updates for population health metrics, and EDI-based data exchange with health plan partners, all running without requiring manual review at each step.
Will MedVision be doing demos at APG Spring Conference 2026?
Yes. The MedVision team will be available for platform walkthroughs and one-on-one discussions at Booth #618 throughout May 27-29. If you'd like to set up a dedicated time before the conference, you can reach out through this link.
Recently published articles
Keep in touch
Subscribe to get the latest update
Trending topics
Share your insights on social media
Upcoming events and company news











