Let’s Discuss Smarter ACO Operations at TXAACOs

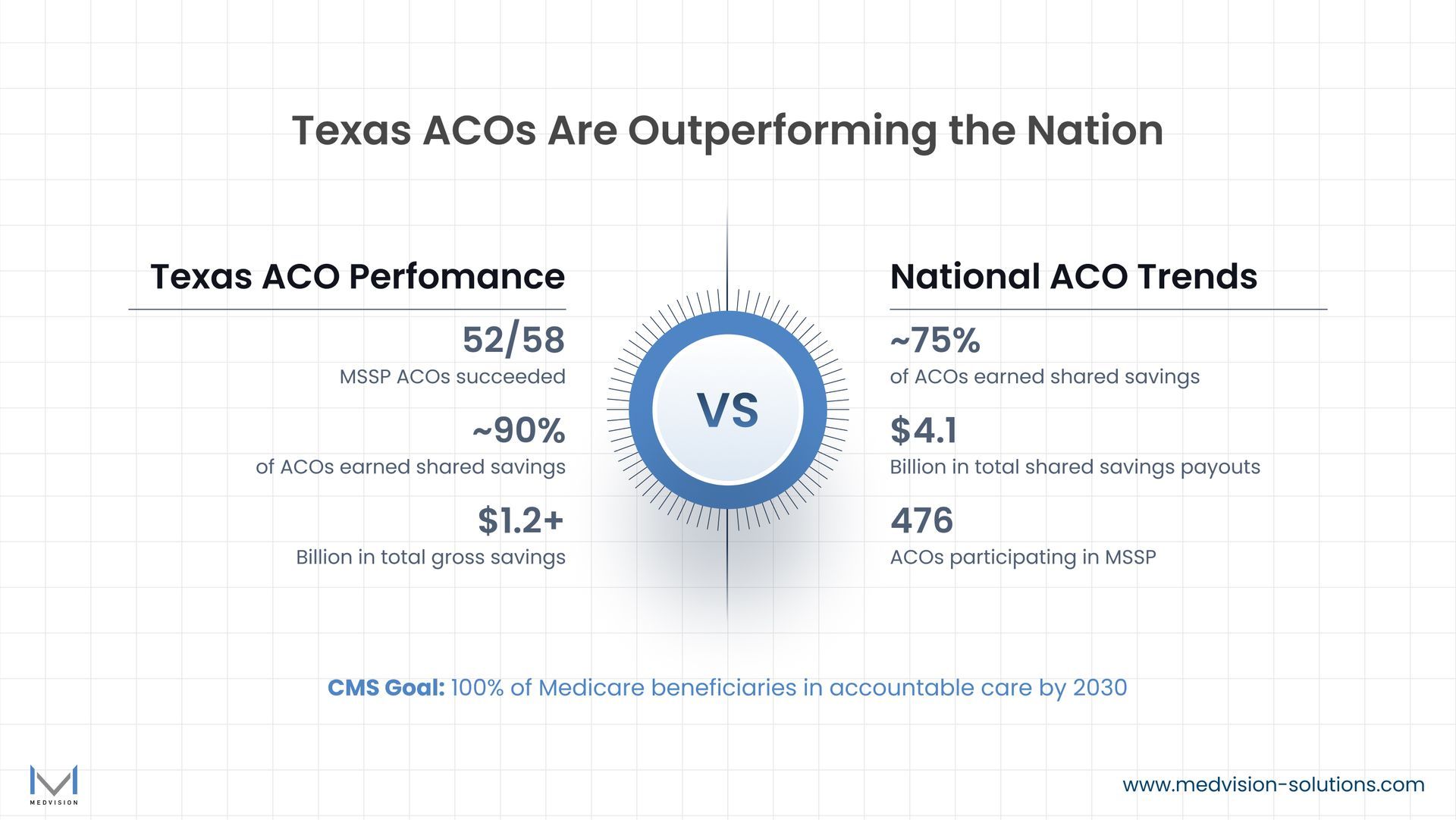
The numbers out of Texas are hard to ignore. In 2024, 52 of the state's 58 MSSP-participating ACOs earned shared savings payments, generating more than $1.2 billion in gross savings combined. Nearly 90 percent of Texas ACOs came out ahead, outpacing the national average by a meaningful margin. That's not a fluke. It reflects what happens when organizations build real operational infrastructure around accountable care, rather than treating value-based care as a checkbox exercise.
If you're heading to the TXAACOs 2026 2nd Annual Spring Conference in Rockwall this May, you already understand that the work of running an ACO has never been more demanding. The benchmarks are tighter. The data expectations are higher. And the organizations pulling ahead are the ones that have closed the gap between clinical intent and administrative execution.
MedVision will be at Booth 15 on May 4-6 at the Hilton Dallas/Rockwall Lakefront, bringing QuickCap 7 to a room full of the people who actually operate Texas's accountable care ecosystem. If you want to see what purpose-built accountable care organization software looks like in practice, that's where we'll be.
ACO Success in Action
Texas ACOs Are Proving the Model Works, But the Pressure Is Real
Texas has become one of the most active ACO markets in the country, with more than 30,000 primary care physicians and nearly 57,000 specialists participating in MSSP ACOs statewide. At the national level, CMS reported in early 2025 that 53.4 percent of traditional Medicare beneficiaries are now in an accountable care relationship, a 4.3 percentage-point jump from the year before and the largest single-year increase since tracking began.
CMS has set a long-term goal of placing all Medicare beneficiaries into accountable care relationships
by 2030. For the ACOs attending TXAACOs this year, that trajectory isn't abstract policy language; it's a mandate with real operational weight.
Earning shared savings isn't simply about providing better care, though that matters enormously. It requires the ability to track quality metrics in real time, manage attributed populations with precision, keep claims clean and timely, and maintain coordination across every stakeholder in the network. Most ACOs today are doing all of that across disconnected systems, and the friction adds up fast.
The Operational Gaps That Hold ACOs Back
The organizations that struggle under value-based care arrangements almost always have the same underlying problem: their administrative infrastructure wasn't built for it.
Fee-for-service workflows don't translate cleanly into shared-savings models. Referral management that worked well in a volume-based environment starts to leak patients and revenue when network integrity becomes a financial variable. Reporting that used to happen quarterly now needs to happen continuously. Risk stratification, once a planning tool, has become a frontline operational requirement.
Fragmented data across multiple systems
When claims data, clinical data, and population analytics live in separate platforms, building a coherent picture of cost and quality becomes extraordinarily time-consuming. The insight you need to intervene early on a high-risk patient often exists somewhere in the system, but getting to it in time is a different challenge.
Manual workflows that create compliance exposure
Authorization management, referral tracking, and claims adjudication done through manual processes are not just inefficient; they introduce errors that affect quality scores, reimbursement, and beneficiary outcomes. In a two-sided risk arrangement, those errors have a direct financial consequence.
Risk adjustment that happens too late
Accurate risk stratification isn't just about documentation and coding. It's about identifying which patients need proactive intervention before their condition escalates into an emergency episode. ACOs that do this well consistently outperform on both cost and quality metrics; those that don't are perpetually reacting rather than managing.
How QuickCap 7 Addresses These Challenges Head-On
MedVision has been building healthcare administration software since 1994. QuickCap 7 (QC7) isn't a general-purpose platform that ACOs are expected to adapt to; it was designed specifically for the operational realities of risk-based and value-based care organizations, ACOs, IPAs, MSOs, TPAs, and the overlapping structures that don't fit neatly into any single category.
Here's what that looks like in practice.
Population Health Management and Risk Stratification
Risk stratification for ACOs is only useful if it drives action. QC7 centralizes your attributed population data and surfaces risk indicators in a format your care management team can actually use. High-risk patients don't get lost in a spreadsheet; they get flagged and tracked. That shift from reactive to proactive care management is one of the clearest ways the right population health management platform improves outcomes at scale.
You can read more about how MedVision approaches ACO population management in our overview of ACO REACH and what it means for risk-based organizations.
Claims Administration and Auto-Adjudication
Clean claims processing is foundational to shared savings performance, and QC7 builds payer-specific rules directly into the adjudication workflow. Rule-based auto-adjudication reduces the risk of fraud, minimizes manual review, and accelerates the revenue cycle without adding headcount. For ACOs managing a large attributed beneficiary population, that kind of throughput consistency matters every single month
Referral Management and Network Integrity
Out-of-network leakage is one of the quieter ways ACOs leave savings on the table. QC7's referral management system provides full visibility into both inbound and outbound referrals, giving your team the tools to keep patients within the network and the care continuum intact. When a referral falls outside the preferred network, your team knows about it in time to act, not after the fact.
Authorization Management with Custom Rules
QC7 allows organizations to create custom rules for authorizations, so the platform reflects your specific clinical and financial policies rather than a one-size-fits-all logic. This reduces manual intervention, speeds up the authorization process, and keeps your utilization management aligned with your quality and cost goals.
Real-Time Dashboards and Quality Reporting
Value-based care administration runs on visibility. QC7's executive dashboards give leadership a real-time window into utilization, cost trends, and quality measure performance, the kind of data you need to make decisions before benchmarks slip. Quality reporting built into the platform means your team spends less time pulling data and more time acting on it.
For a closer look at how integrated technology changes ACO performance, see our piece on
what complete health solutions mean for accountable care organizations.
What TXAACOs 2026 Represents for the Accountable Care Community in Texas
The 2nd Annual TXAACOs Conference isn't just a networking event. It's the gathering point for the people actively building Texas's accountable care infrastructure: ACO leaders, MSO operators, clinical directors, and administrators who are working through the same challenges and looking for answers that actually translate into practice.
This year's conference at the Hilton Dallas/Rockwall Lakefront brings that community together against the backdrop of a genuinely pivotal moment in the MSSP landscape. CMS is accelerating the push toward two-sided risk arrangements.
The ACO REACH model, which runs through 2026, is transitioning to the LEAD Model in 2027, a 10-year initiative that will reshape how advanced risk-based organizations operate. Texas ACOs are already navigating this transition while simultaneously managing a growing beneficiary population and increasingly sophisticated quality benchmarks.
That's the conversation MedVision wants to be part of at Booth 15.
Our team will be available throughout the conference for one-on-one conversations and platform demos. Whether you're evaluating ACO management software for the first time or looking to replace a system that's reaching its limits, we're there to talk through what QuickCap 7 would look like for your specific organizational structure.
Coming to TXAACOs 2026? Here's How to Find Us
Event: 2nd Annual TXAACOs Conference
Dates: May 4-6, 2026
Location: Bella Harbor Ballroom A/B/C and Pre-Function North/West
Hilton Dallas/Rockwall Lakefront
2055 Summer Lee Drive, Rockwall, TX 75032
MedVision Booth: 15
The conference brings together ACOs, healthcare innovators, clinicians, and policy leaders from across Texas and beyond. If accountable care is part of how your organization operates, this is the room to be in.
We're looking forward to the conversations. Stop by Booth 15 anytime during the event or explore our ACO solutions page ahead of time to get a sense of what we'll be walking you through.
Talk to Us at Booth 15
Frequently Asked Questions
What is ACO management software, and how is it different from a standard EHR?
A standard EHR focuses on clinical documentation and patient records. ACO management software goes further, integrating clinical data with financial and administrative workflows, including claims adjudication, referral tracking, authorization management, and quality reporting. It's designed to support the operational demands of risk-based and value-based arrangements, not just clinical care delivery.
How does risk stratification for ACOs improve shared savings performance?
Risk stratification for ACOs helps care management teams identify high-need patients before they generate high-cost episodes. By surfacing risk indicators early and routing those patients into proactive intervention programs, ACOs can reduce unnecessary hospitalizations and emergency visits, two of the most significant drivers of cost overruns against shared savings benchmarks.
What does a population health management platform actually do for day-to-day ACO operations?
A population health management platform centralizes attributed beneficiary data, tracks quality metrics across the population, and gives administrators real-time visibility into where care gaps exist. In practical terms, it means your team spends less time searching for information and more time acting on it, which translates directly into better quality scores and stronger financial performance.
Will MedVision be doing demos at TXAACOs 2026?
Yes. The MedVision team will be available for platform walkthroughs and one-on-one conversations at Booth 15 throughout May 4-6. If you'd like to set up a dedicated time before the conference, you can reach out through the QuickCap solutions page.
Recently published articles
Keep in touch
Subscribe to get the latest update
Trending topics
Share your insights on social media
Upcoming events and company news











